Memory Deficit Syndromes
Memory Deficit Syndromes are progressive neurological conditions characterized by impaired ability to encode, store, or retrieve information due to synaptic dysfunction or neurodegeneration. Affecting tens of millions worldwide—a number rising with population aging—these disorders profoundly impact quality of life, independence, and emotional well-being. Current treatments provide only limited symptomatic relief without halting disease progression, creating an urgent unmet need for novel therapies that can restore cognitive function.
About Memory Deficit Syndromes
Memory Deficit Syndromes are chronic neurological disorders that manifest through progressive cognitive decline, specifically the impairment of the ability to encode, store, or retrieve information. While the clinical presentation often involves amnestic syndromes—ranging from mild forgetfulness to profound loss of self-identity—the underlying causes are diverse.
The complexity of these syndromes arises from distinct pathological mechanisms that damage critical brain networks. The most common etiologies include:
- Neurodegenerative Diseases: Primarily Alzheimer’s Disease and Lewy Body Dementia, where abnormal protein deposits (such as amyloid plaques and tau tangles) cause irreversible neuronal death and synaptic loss.
- Cerebrovascular Pathology: Conditions like Vascular Dementia, resulting from strokes or chronic small vessel disease that disrupt blood flow and oxygen supply to memory centers.
- Traumatic Brain Injury (TBI): Physical damage to brain structures from acute accidents or repetitive impacts, leading to disruption of neural circuits and axonal injury.
- Metabolic & Nutritional Imbalances: Reversible or progressive deficits caused by factorssuch as vitamin B1 (thiamine) and B12 deficiency, hypothyroidism, and hepatic or renal encephalopathy.
- Other Causes: Aging-related synaptic dysfunction, viral encephalitis, psychiatric conditions…
Memory Deficit Syndromes affect more than 55 million people worldwide, significantly impacting their quality of life. Each year, nearly 10 million new cases are diagnosed. The nature of the deficits is heavily influenced by these specific etiologies, leading to varied manifestations ranging from episodic memory lapses to disruptions in semantic knowledge and spatial navigation.
Current Treatment
The management of Memory Deficit Syndromes is currently limited and primarily focuses on symptomatic relief rather than curative intervention. Treatment strategies are stratified by etiology:
- Pharmacological Interventions: The standard of care for neurodegenerative forms (e.g., Alzheimer’s disease) relies on cholinesterase inhibitors and NMDA receptor antagonists. While these agents can temporarily stabilize cognitive function by enhancing neurotransmission, they do not arrest the underlying pathological progression. Recently approved anti-amyloid immunotherapies offer disease-modifying potential for specific subsets of patients but are associated with significant safety monitoring requirements and variable clinical efficacy.
- Vascular & Metabolic Management: For non-neurodegenerative causes, treatment prioritizes the control of risk factors, such as hypertension, diabetes, and lipid profiles, to prevent further cerebrovascular injury and optimize brain metabolism.
- Supportive Therapies: Cognitive rehabilitation and lifestyle modifications serve as adjunctive measures to maintain functional independence.
Despite these available options, a profound therapeutic gap remains. There are currently no approved therapies capable of restoring lost synaptic connections or reversing established memory deficits, underscoring the urgent need for novel regenerative and neuroprotective agents.
Novel Approch for the Treatment
Neu-003 is a novel, orally bioavailable small molecule designed to target the core synaptic deficit underlying memory impairment. Unlike conventional symptomatic therapies that modulate neurotransmitter levels, Neu-003 directly enhances long-term potentiation (LTP)—the fundamental cellular mechanism of learning and memory—offering a differentiated, mechanism-driven approach to treating Memory Deficit Syndromes.
In ex vivo electrophysiology studies, Neu-003 induced robust cortical LTP in wild-type mouse brain slices at nanomolar concentrations (200–500 nM, ****p < 0.0001), demonstrating potent and dose-dependent enhancement of synaptic strength
When administered orally to aged triple-transgenic Alzheimer’s disease (3×Tg AD) mice—a well-established model recapitulating amyloid, tau, and synaptic pathology—Neu-003 produced striking cognitive restoration across multiple behavioral paradigms
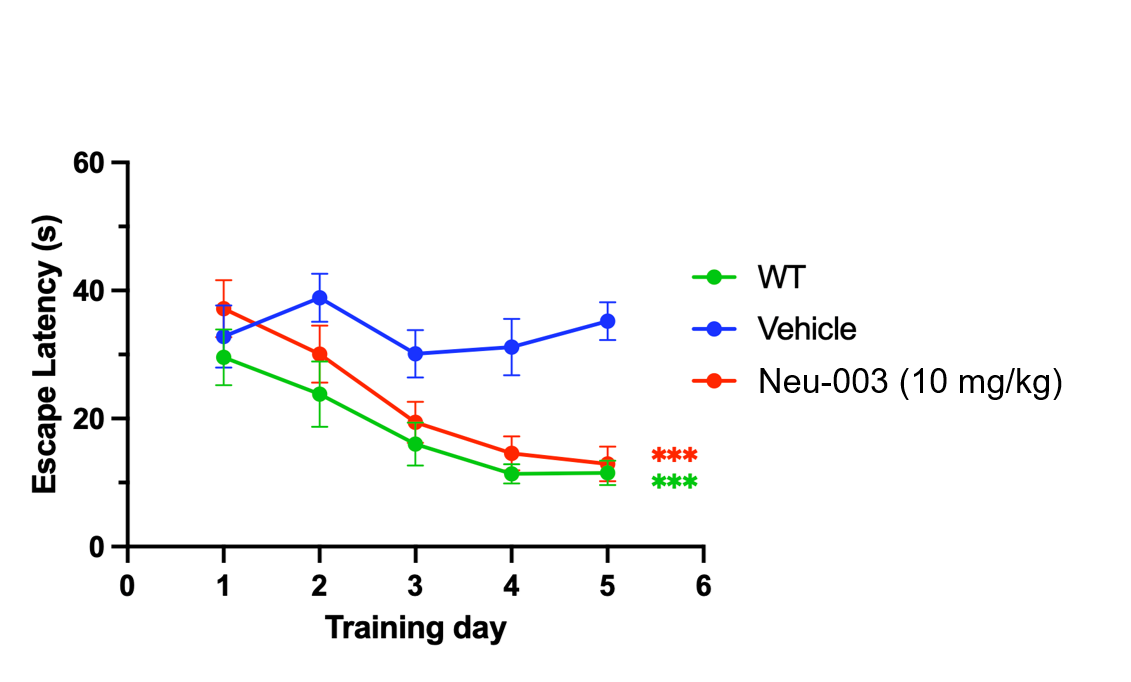
Learning Restored
Neu-003-treated AD mice acquired spatial memory at the same rate as wild-type controls over 5 days of training (p < 0.001 vs. vehicle).
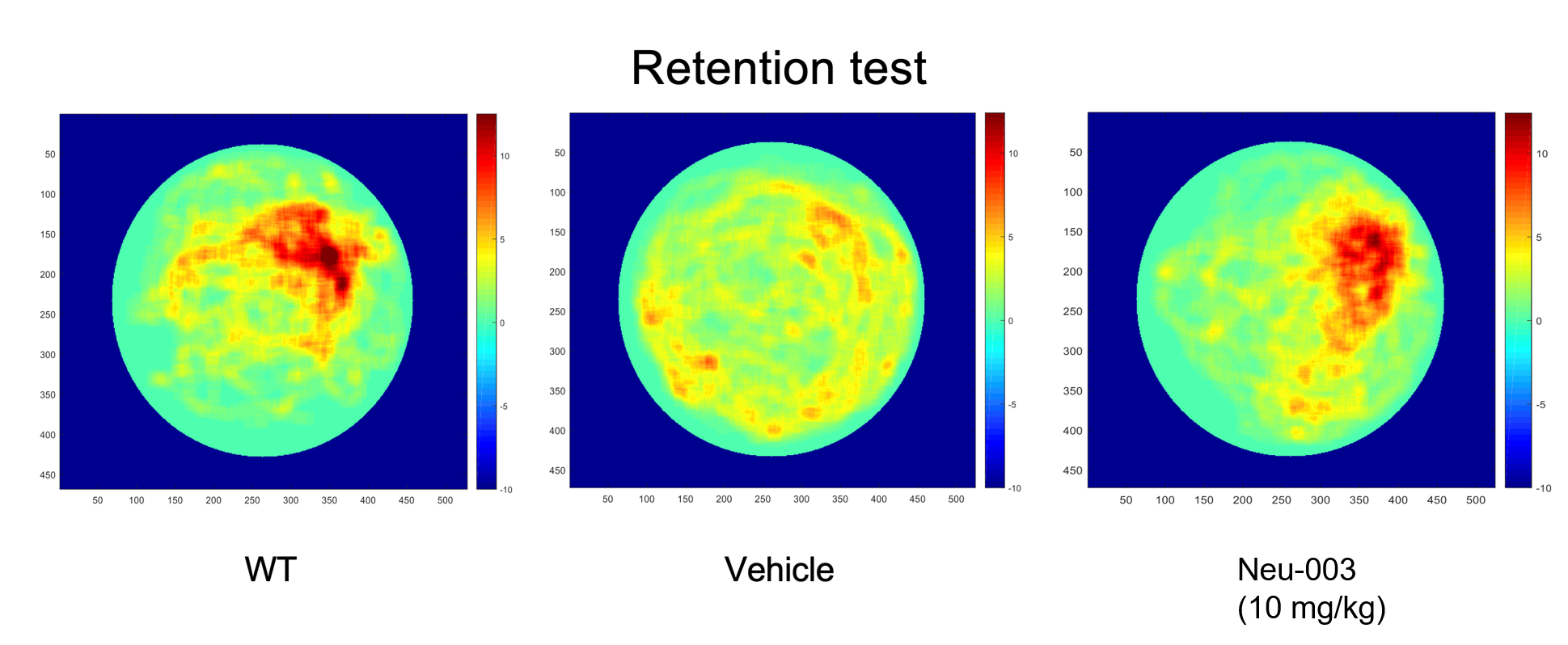
Memory Retained
In the probe trial, treated animals spent significantly more time in the target quadrant and made more platform crossings than vehicle-treated AD mice, matching wild-type performance.
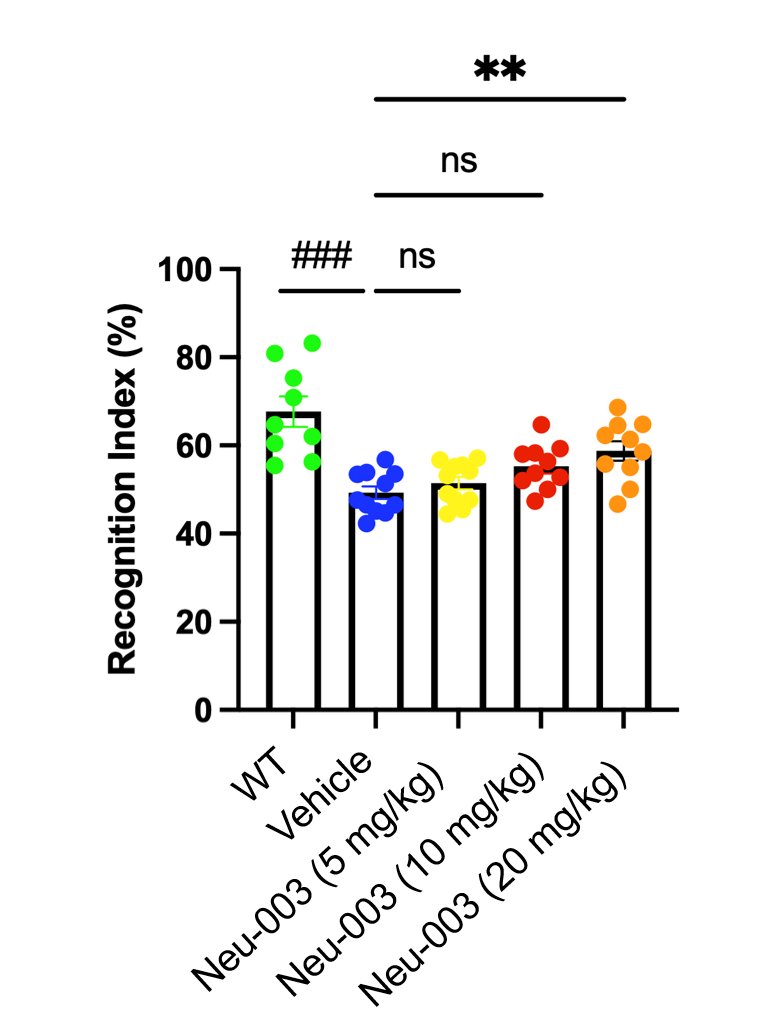
Recognition Enhanced
In the Novel Object Recognition test, a single dose of Neu-003 (20 mg/kg, i.p.) significantly improved the recognition index in aged AD mice (**p < 0.01), confirming pro-cognitive effects across independent memory domains.
Together, these data demonstrate that Neu-003 not only enhances the biological substrate of memory at the synaptic level but also translates into meaningful cognitive improvement in a disease-relevant animal model. As an orally available agent with a novel mechanism of action, Neu-003 represents a promising therapeutic candidate poised to address the critical unmet need in Memory Deficit Syndromes.

